The Affordable Care Act (ACA) requires employers to provide timely, affordable, and minimum-value health coverage to their workforce. However, providing adequate coverage is only half the equation. To satisfy ACA reporting compliance and prevent penalty assessments, employers must meticulously track workforce data and consistently prove their compliance each tax year.
This toolkit breaks down the complexities of the Employer Mandate, core 1095-C reporting rules, and proactive compliance strategies.
What is ACA Reporting Compliance?
ACA compliance is the federal requirement for large employers to offer affordable, minimum-value health insurance to their full-time employees or face IRS tax penalties.
Specifically, under the ACA’s Employer Shared Responsibility Payment (ESRP) mandate, businesses must offer health insurance that provides Minimum Essential Coverage (MEC) and Minimum Value (MV) to at least 95% of their full-time workforce and their dependents.
To prove you have met these ACA requirements, you must provide employees with Form 1095-C and file Forms 1094-C and 1095-C with the IRS (and applicable state agencies) annually. If the data submitted is inaccurate, late, or shows a failure to offer adequate coverage, the IRS will issue penalty notices.
Who Must Comply with the ACA?
The health insurance mandate applies to Applicable Large Employers (ALEs).
An ALE is any organization that employed an average of 50 or more full-time or full-time equivalent (FTE) employees during the previous calendar year.
- Important Note: Businesses sharing a common owner with multiple Federal Employer Identification Numbers (FEINs) are not counted separately. They are grouped together as related entities to determine ALE status.
The 3 Core ACA Reporting Compliance Requirements
Successful Affordable Care Act tracking requires year-round attention to three critical areas:
- Determining Employee Eligibility: Traditional HR titles do not dictate ACA eligibility. Under the ACA, a full-time employee is anyone who averages 30+ hours per week or 130+ hours per month. Employers must continuously track workforce hours, including leaves of absence, to know exactly who requires an offer of coverage.
- Confirming Affordability: An employer-sponsored health plan cannot cost an employee more than a specific percentage of their household income. Because employers rarely know an employee’s total household income, the IRS provides three (W-2 wages, Rate of Pay, and Federal Poverty Line) to help organizations set and prove affordable premium contributions.
- Reporting the Data: Employers must file Forms 1094-C and 1095-C with the IRS and furnish 1095-Cs to employees. Recent IRS updates allow furnishing 1095-Cs only upon request (with proper notification), alongside traditional mail or electronic delivery. Note that state mandates in CA, NJ, RI, and D.C. often still require automatic, standard furnishing.

Understanding ACA Reporting Compliance Penalties
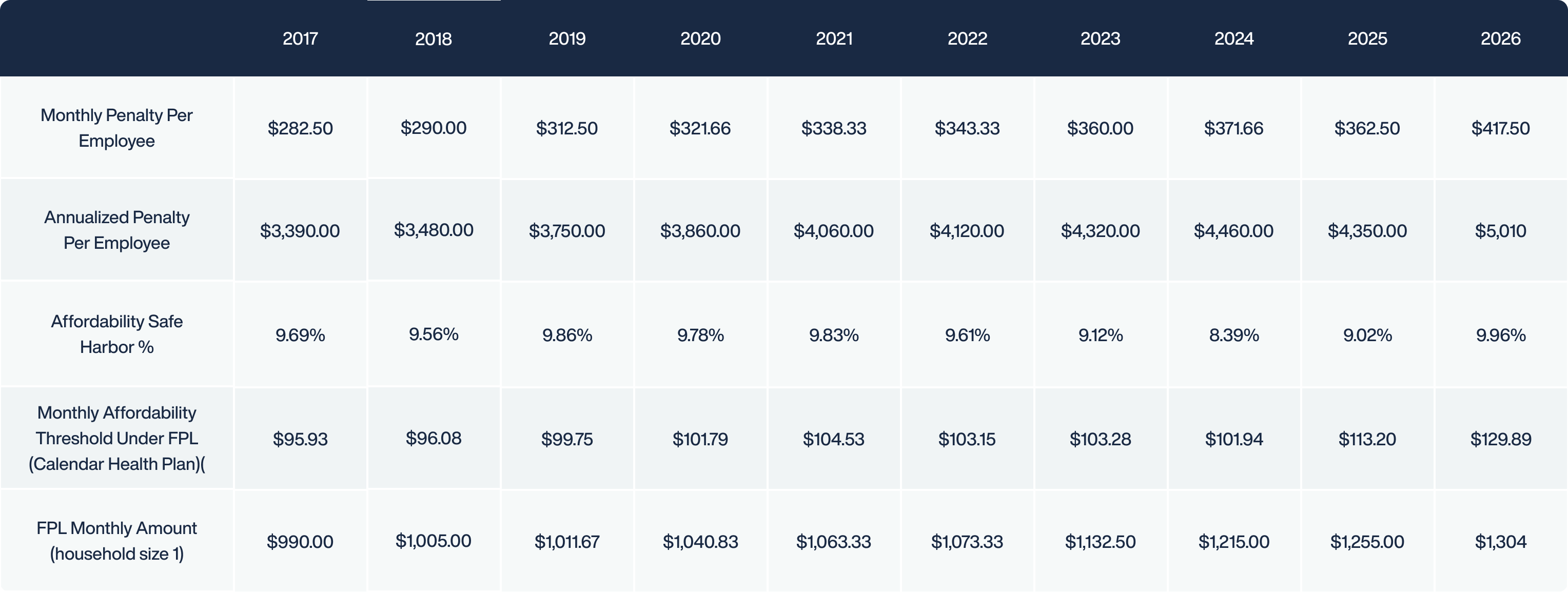
The IRS enforces the ACA strictly. If you fail to meet the requirements, you may be subject to the following assessments (rates below reflect the 2025 tax year):
- Failure to File/Furnish (IRC 6721 & 6722): Penalties assessed per individual return for failing to provide employees with correct statements or failing to file accurate returns with the IRS by the mandated deadlines.
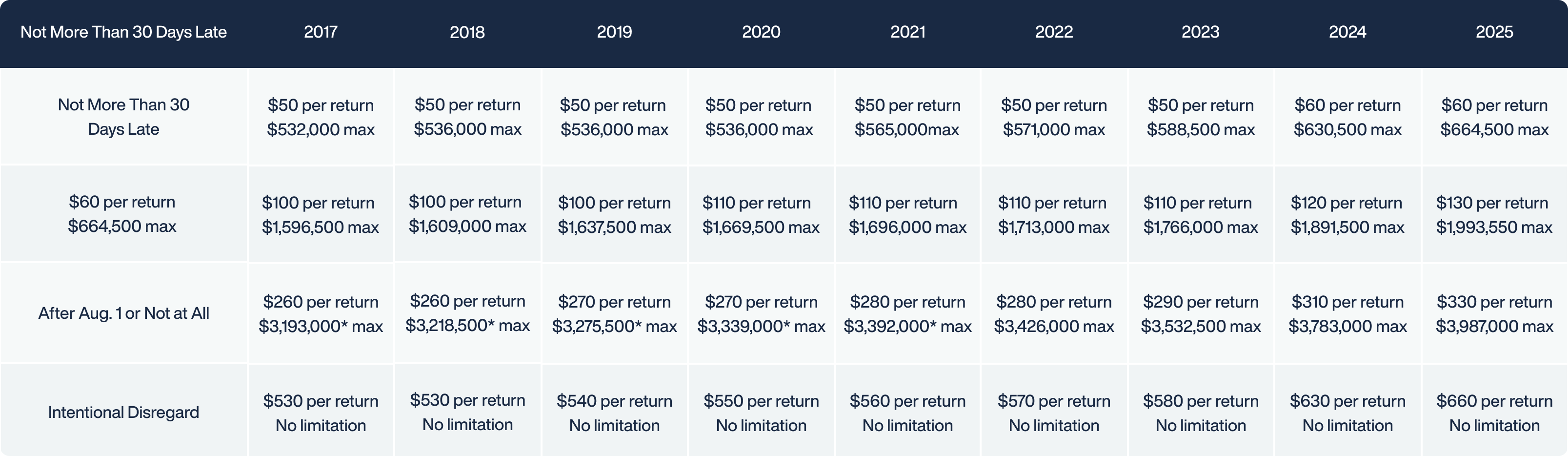
- The “A” Penalty (IRC 4980H(a)): Triggered if an employer fails to offer Minimum Essential Coverage to at least 95% of its full-time workforce, and at least one employee receives a Premium Tax Credit (PTC) from a state exchange. (2025 Penalty: $2,900 annually per full time (non-limited non assessment period) employee, minus the first 30).
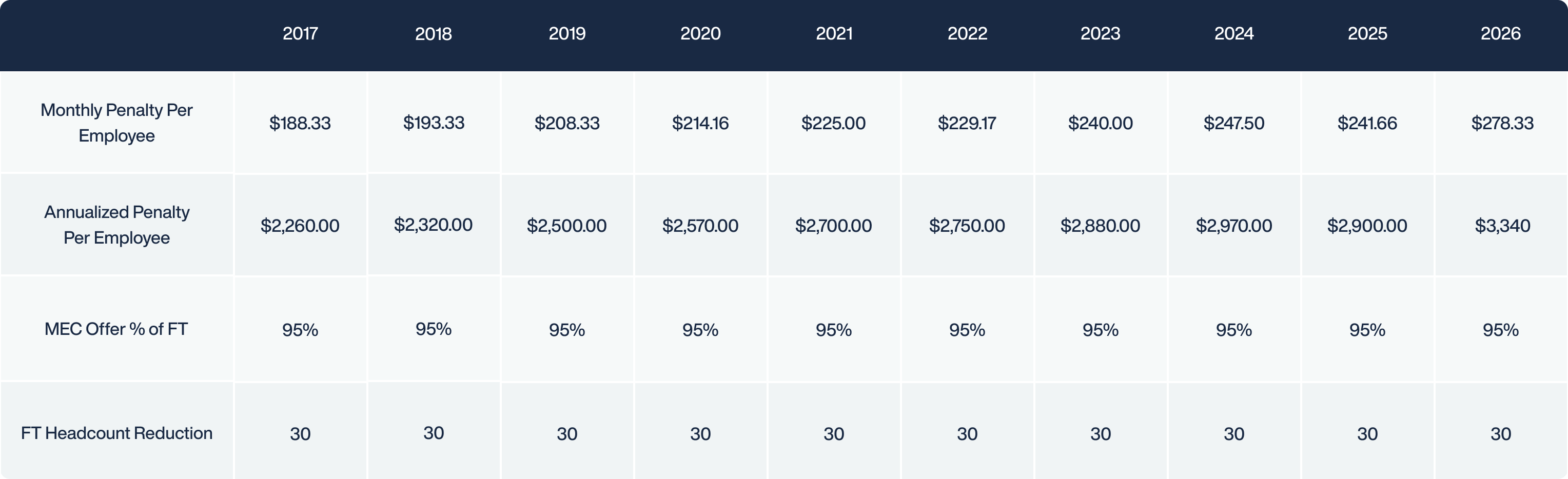
- The “B” Penalty (IRC 4980H(b)): Triggered if an employer offers coverage, but it is either unaffordable or does not provide Minimum Value, and an employee subsequently receives a PTC. (2025 Penalty: $4,350 annually per employee receiving a subsidy).
The IRS Penalty Letter 226J Process
If the IRS detects non-compliance, they will initiate the penalty assessment process via Here is what to expect:
- Receipt of Letter 226J: Includes a summary of the proposed penalty and a list of employees who received a PTC. You have 90 days to respond.
- Form 14764 ESRP Response: The formal document used to agree with or contest the proposed penalty.
- Letter 227: The IRS acknowledgment of your response, outlining the next steps.
- Pre-Assessment Conference: If you disagree with Letter 227, you may request a conference with the IRS Office of Appeals within 30 days.
- Notice CP 220J (Demand of Payment): The final notice requiring payment, issued after the appeals process or if an employer fails to respond entirely.
How to Simplify ACA Reporting Compliance: The Monthly Review
The most common mistake employers make is treating the ACA as a year-end, annual tax exercise. Because the IRS assesses penalties based on monthly employee data, the best way to fortify your ACA compliance process is to conduct a monthly ACA compliance review.
At Trusaic, we secure employer compliance using the Triangle of Trust™:
- Data Quality Management: The analytical outputs on your 1095-C forms are only as good as the raw HR, payroll, and benefits data fed into them. Aggregating siloed data into a single source of truth prevents the formatting errors that trigger audits.
- Analytics: Once data is consolidated, it must be analyzed to accurately calculate hours of service, track measurement periods, and apply affordability safe harbors correctly.
- Regulatory Expertise: Do-it-yourself ACA reporting software packages will auto-populate IRS forms regardless of whether the data makes sense. You need expert human oversight to interpret the regulations, apply Limited Non-Assessment Periods, and ensure audit-ready documentation.
5 Common ACA Compliance Mistakes
1. Overlooking Aggregated Employer Group Rules
Failure to accurately group related entities is a frequent trigger for IRS penalties. While an individual organization might not meet the 50-employee threshold to be considered an Applicable Large Employer (ALE) on its own, businesses sharing common ownership must be aggregated. If the combined workforce meets the ALE threshold, all entities within the group are subject to the Employer Mandate and its reporting requirements.
2. Applying the Wrong IRS Measurement Methodology
The IRS provides two distinct methods for determining an employee’s full-time status: the Monthly Measurement Method and the Look-Back Measurement Method. Selecting the wrong methodology for a specific workforce — particularly those with highly variable or seasonal hours — often leads to inaccurate eligibility calculations, missed offers of coverage, and subsequent penalty assessments.
3. Misclassifying Employee Status
Traditional HR job titles do not dictate ACA eligibility. The IRS maintains strict, specific definitions for full-time, part-time, variable-hour, and seasonal employees. Misclassifying a worker’s status can cause an employer to inadvertently exclude eligible employees from health plan offers, directly exposing the organization to IRC 4980H penalties.
4. Failing to Track Service Breaks and Transition Dates
Accurate ACA reporting requires precise, month-by-month tracking of an employee’s hours of service. Failing to properly document critical transition dates — such as initial hires, rehires, terminations, and extended leaves of absence (like FMLA) — can distort full-time status calculations and result in flawed Form 1095-C coding.
5. Disconnecting Health Benefit Data from Payroll Data
ACA compliance requires a holistic view of both workforce hours and benefit offerings. Employers frequently err by failing to properly substantiate the cost of their health plans against employee wages.
To prove compliance, organizations must maintain audit-ready documentation detailing plan affordability, Minimum Value (MV), enrollment timelines, and how complex arrangements like opt-out payments or health reimbursement arrangements (HRAs) impact the employee’s required premium contribution.
Take the Stress Out of ACA Season with Trusaic
From seamless data integration to complex penalty defense, Trusaic’s ACA Complete® platform handles the heavy lifting so your HR team doesn’t have to. Stop wrestling with spreadsheets and ensure your data is accurate, affordable, and filed on time.